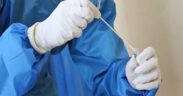
A shortage of ventilators will put lives in danger, so health authorities round the world do everything they will to urge more
Health authorities round the world try to search out ways to fill their hospitals with more ventilators to address increasing numbers of coronavirus patients.
While the overwhelming majority of individuals who catch the Covid-19 disease experience only mild symptoms, about 6% need medical care, with older patients at higher risk.
Australian authorities say they’re confident they will avoid any shortage of ventilators.
Experts have told Guardian Australia that these efforts are going to be crucial, because a shortage of ventilators would put lives in danger.
“The reason this can be a crisis is because without the ventilators, patients will die,” says Prof David Story, deputy director of the University of Melbourne’s Centre for Integrated Critical Care, and a staff anaesthetist at Austin Hospital.
What is a ventilator and the way does it work?
A mechanical ventilator could be a machine that’s wont to support patients with severe respiratory conditions that impact the lungs, including pneumonia.
Before a patient is placed on a ventilator, Day says medical staff – often anaesthetists – will perform a procedure called intubation.
After a patient is sedated and given a relaxant, a tube is placed through the mouth and into the windpipe.
Day says the procedure is routine but, with Covid-19 patients, medical staff must take extreme precautions to create sure they are doing not become infected with the virus.
“We have people almost fully hazmat suits,” he says.
The breathing tube is then attached to the ventilator and medical staff can adjust the speed that it pushes the air and oxygen into the lungs, and adjust the oxygen mix.
When would a patient go onto a ventilator?
Before deciding to place a patient onto a ventilator, Story says doctors are searching for signs of “respiratory failure”.
“The breathing rate will increase, they’ll look distressed, the CO2 within the blood goes up and that they can become sedated and confused,” he says.
He says while a standard breathing rate is about 15 breaths a second, if the speed gets to about 28 times a second, then this can be a proof that ventilation is also needed.
Before happening a mechanical ventilator, Prof John Wilson, president-elect of the Royal Australasian College of Physicians and a respiratory physician, says there is also other attempts to extend a patient’s oxygen levels.
These “non-invasive” methods of ventilation can include masks and oxygen tanks.
Story says that with Covid-19, medical staff were looking to avoid non-invasive methods because patients would still cough and splutter, increasing the danger of the virus being transferred to medical staff.
How soon might a patient need a ventilator and for a way long?
Ranganathan says once a doctor sees that a patient needs a ventilator, “it is required quickly”.
He says: “The patient are often sustained for brief periods of your time using manual styles of ventilation like employing a bag and mask system with oxygen, but usually being attached to a ventilator must happen within half-hour if critical.”
Story says that in severe Covid-19 patients, a life-threatening condition can develop called acute respiratory distress syndrome (Ards) that needs ventilators to deliver smaller volumes of oxygen and air, but at higher rates.
This could mean a patient may have to air a ventilator “for weeks”.
To avoid complications from the breathing tube happening the throat, Story says a tracheostomy is applied that the tube can go straight into the windpipe through the neck.
“Patients are often more awake with tracheostomy and also the hole just heals itself,” says Story.
“If patients develop Ards they’ll be in an medical aid unit for weeks and they’ll die without ventilators.”
Why a shortage of ventilators matters, and what’s being done to avoid it.
One of the foremost obvious ways to avoid a shortage of ventilators, is to scale back the numbers of individuals catching the disease within the first place. meaning following all the health advice, including social distancing and hygiene rules.
In Australia, the Australian Healthcare and Hospitals Association, the Australia and New Zealand medical aid Society and also the industry minister, Karen Andrews, have all expressed confidence that a shortage are often avoided.
Source: The Guardian