New guidance from the World Health Organization (WHO) and the International Atomic Energy Agency (IAEA) on the procurement of radiotherapy equipment could improve access to this life-saving cancer treatment option that is still lacking in many parts of the world.
The new technical guidance aims to ensure that the selection of radiotherapy equipment is appropriate to country and health facility contexts, that treatment is delivered safely, that quality is maintained, and that services are sustainable.
The publication is intended for medical physicists, biomedical and clinical engineers, radiation oncologists, oncologists and anyone else with responsibility for manufacturing, planning, selecting, procuring, regulating, installing or using radiotherapy equipment. It was developed as part of the ongoing collaboration between WHO and the IAEA to foster safety and quality in the medical use of radiation technology.
More than half of cancer patients require radiotherapy
More than 50% of cancer patients require radiotherapy as part of cancer care and it is frequently used to treat the most common types, such as breast, cervical, colorectal, and lung cancer. Yet, access to radiotherapy is inadequate, particularly in low- and middle-income countries.
“IAEA data shows that around one-third of countries still do not have radiotherapy available, out of which 28 are in Africa,” said May Abdel-Wahab, Director of the IAEA’s Division of Human Health. “Many of them would benefit from increased access to radiotherapy services. The key is tailoring radiation oncology solutions to the situation on the ground, underpinned by appropriate safety infrastructure.”
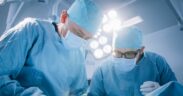
Types of radiotherapy equipment covered by the guide include external beam radiotherapy machines (both Cobalt-60 and linear accelerators), brachytherapy devices that apply radiation sources directly to tumours and complementary imaging devices such as conventional or computed tomography (CT) simulators, as well as other tools essential for safe operation and quality control. Depending on the type of radiotherapy machine, the need for specialized professionals and infrastructure, as well as quality assurance and maintenance, may vary.
Safety is also covered extensively, with information provided on planning for bunkers to house radiotherapy equipment, shielding for walls, floor and ceilings and emergency buttons for treatment and control rooms. In addition, clear guidance is provided on what is required to ensure functionality of equipment for an optimal equipment lifespan, usually a period of 10-15 years.
Selecting radiotherapy systems appropriate for given settings and matched to the existing workforce help ensure the delivery of safe radiotherapy. It contributes to the improvement of access to life-saving treatment by minimizing service interruptions because of machine downtime and builds a solid foundation for further expansion of services when the health-care system is ready for adoption of more complex radiotherapy systems.
“While interruptions of radiotherapy equipment predate COVID-19,” said Dr Bente Mikkelsen, Director of the Department of Noncommunicable Diseases at WHO, “they have been exacerbated during the pandemic because of breakdowns in global supply chains and barriers to the free movement of technical service personnel. Any improvement that reduces interruptions can make the difference between life and death for patients whose tumours continue growing while they await treatment.”
Radiotherapy equipment is, however, just one element of cancer management services. Others that need to be in place relate to early detection, diagnostic imaging, laboratory testing, pathology, surgery, systemic treatment and palliative care. The technologies associated with all of these services are listed in the WHO List of Priority Medical Devices for Cancer Management.
Global cancer initiatives
One area where radiotherapy plays an important role is in curing cervical cancer, one of the leading causes of cancer deaths among women, and for which WHO launched a global elimination strategy last year.
“Cervical cancer is curable if we catch it early,” said Dr Nono Simelela, WHO Assistant Director-General for Strategic Priorities. “We have the tools to save lives. Radiotherapy is one of them. It is also one of the most effective tools to mitigate pain and suffering associated with advanced cancers.”
Unitaid, a global health agency engaged in finding innovative solutions to prevent, diagnose and treat major infectious diseases in low- and middle-income countries, has recently expanded its portfolio to include HIV co-morbidities, such as cervical cancer. “While Unitaid’s catalytic investments have targeted cervical cancer screening programmes, critical functions such as radiotherapy procurement represent an important component of the continuum of care for any women in need of invasive cancer treatment,” said Robert Matiru, Director of Unitaid’s Programme Division.
Radiotherapy is also an integral part of breast and childhood cancer control, two other major WHO global cancer initiatives. The changes that will be facilitated by the new guidance will also benefit millions of cancer patients globally, including women seeking treatment for breast cancer, now the most commonly-diagnosed form of cancer globally.
The new specifications are an update of a previous version issued by the IAEA, published in 2008.
Note for journalists:
WHO supports countries in strengthening their national cancer control policies and health-care systems, ensuring appropriate priority setting and the establishment or scaling-up of accessible, equitable and quality cancer care as part of universal health coverage. WHO’s cancer focus is on childhood, cervical and breast cancers.
The IAEA supports countries in the use of nuclear and radiation medicine to fight a range of noncommunicable diseases, including cancer. The Agency supports countries in resource mobilization and the procurement of equipment, as well as through training, education, research, guidance documents and in carrying out quality assessments and missions.
Based on a city where the mountain meets the sea and where antique houses line the streets, my mind is free to wonder, to wander and to write.