Should the NHS prioritize patient outcomes above financial performance, access and addressing health inequalities? For this article I have replaced inequalities with inequities. While inequality is a significant, the real issue for many health systems is inequity.
Increasingly, those responsible for managing today’s health systems are retreating from the idea that achieving all three objectives is not possible and trade-offs between them are becoming the norm.
How did we get to this point?
The graph below provides a useful insight into how we got to this point.
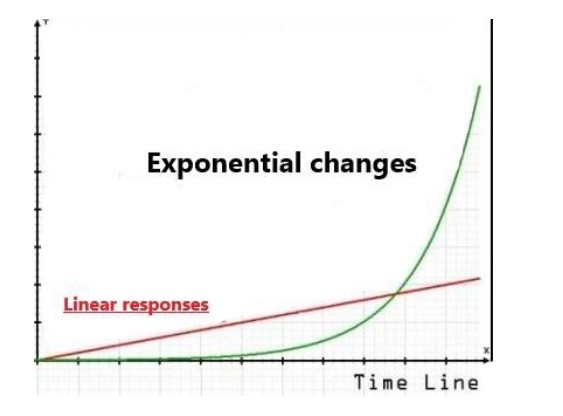
In simple terms, it is the story of changes in demand and supply moving at a different pace. Changes in demand are moving along on the exponential curve while health system supply responses continue to change on the linear line.
The narrative of this graph has two parts:
- Part 1 – where supply responses exceeded demand expectations. Advances in public health, prevention programmes, the introduction of new diagnostic and screening programmes, the breakthrough in new therapeutic medicine and novel treatment techniques throughout the 20th century has been a significant reason for increasing human life expectancy.
- Part 2 – where demand has exceeded supply. This is today’s 21st-century reality for many First world health systems. This growing chasm is the domain of widening inequities, growing fiscal deficits, uneven and potentially poor health outcomes.
Demand
Demand-side changes, moving on an exponential curve trajectory driven by the speed, volume, frequency, and convergence include:
- Demographic and social changes
- Environmental (physical and climatic) changes
- Scientific, engineering and technology changes
- Political and economic changes
The complexity, uncertainty, and ambiguity of these changes make it challenging to respond traditionally. The consequence and impact on individuals, families, communities, and population have become difficult to predict. The recent forest fires in California with its devastating impact is a case in point.
Many of these changes in its early stages to the casual observer look very benign and inconsequential. However, its exponential trajectory will accelerate to a “J” or “hockey stick” point. When that happens demand changes will quickly catch up with any slag in the supply line, cross the “tipping point” before racing ahead and opening the gap between the two.
Stephen Kotler’s concept of 6Ds
Stephen Kotler’s concept of 6Ds (digitalization, democratization, demonetization, deception, and disruption) provides one of the better explanations on why the exponential curve behaves this way. The book BOLD by Stephen and Peter Diamantis provides a good explanation of the impact of the 6Ds.
Supply
Supply responses contributing to this gap include:
- Discovery, trials, development, adoption cycle takes too long and too expensive.
- Fixed and static facilities dominate health service delivery practices.
- Cottage industry or industrial era practices dominants health service delivery, organization, business, and management models.
- Workforce training and development emphasized specialization, takes a long time and done in silos — challenges in maintaining up-to-date skills and knowledge driven by rapid changes in science and technology.
- Policy, regulatory practices, funding and investment models heavily weighted toward maintaining the status quo with insufficient sustainable incentives to stimulate innovations.
- Integration difficulties are reinforcing fragmented health services.
What is the way forward?
Leading, managing and changing responses in an environment of exponential change requires more than better strategy, tools, and resources. It needs leaders that can create a team-based culture and environment that is comfortable with constant change, prepared to take a safe to fail (early, fast and inexpensive) portfolio approach to innovation and courageous to make swift decisions (stop, accelerate or change) on current core activities.
Crossing the chasm to deliver on all three objectives requires the following 7 pieces of the jigsaw:
- Change in mindset – from deficit to abundance, from risk to opportunities, from failure to learnings, from “me” to “us” and from “yes but” to “yes and.”
- System approach to a dual transformation change programme.
- Integrated change framework to execute the change.
- Different capability, capacity, skills, and knowledge for each part of the dual transformation.
- Open, learning, team-based and courageous culture.
- Keeping pace with changes in external environment.
- Making changes internally to be ahead of external environment changes.
Final remarks
The three objectives of “better outcomes, reducing inequities and balancing the books” is the high–water mark for any health system. Today’s ever-growing and deepening chasm between the exponential forces that drive demand and the linear pace of responses has given rise to a mindset that all three cannot be achieved. Trade-offs between them must be made. This is flawed thinking and is an admission that the pressure has got the better of us. This flawed position is also contributing, reinforcing and deepening the chasm.
The alternative and only viable view is to not just cross the chasm but always to be ahead of the demand curve so that ALL three objectives are a reality. The transition phase may see uneven progress, but the trend of improvements for all three objectives remains positive. Keeping the balance and ensuring that no one objective is lagging too far behind is first and foremost a leadership challenge.
Many government committees, boardroom, and senior executive‘s agenda give an insight of where they are on this leadership challenge. There are glimpses of progress but there remains a lot of ground to be covered. When you read this article, where are you and your organization in this leadership challenge? Reflect on where you and your organisation are currently position on the exponential/linear graph and against the 7 pieces of the jigsaw puzzle. History are made and futures shaped by those who embrace and execute all 7 pieces of the jigsaw!






















